Foot Health Blog
Find expert articles from physical therapists and podiatrists to help understand, diagnose, and treat different foot health issues such as plantar fasciitis, bunions, flat feet, and more.
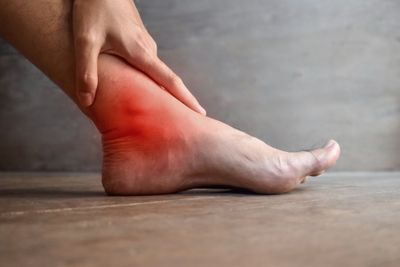
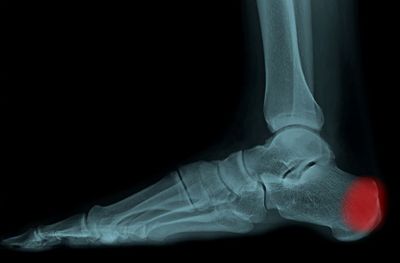
Achilles tendonitis
Achilles Tendinopathy vs. Tendonitis: Differences and DefinitionsTendinopathy and tendonitis are two types of Achilles tendon pain and are often confused as their symptoms are extremely similar, and the injury occurs in the same region. Both conditions cause pain aDecember 19, 2024
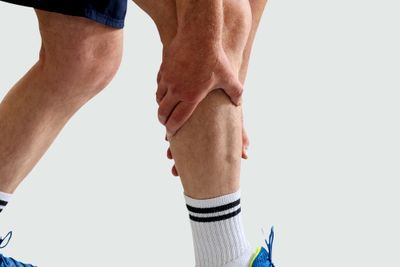
Achilles tendonitis
Preventing Achilles Tendonitis: 5 Strategies That Are Vital to KnowAchilles tendonitis is a common cause of pain in the lower limbs, especially among runners. The condition occurs when the Achilles tendon becomes inflamed and is often associated with overuse.
There January 30, 2024